[ad_1]
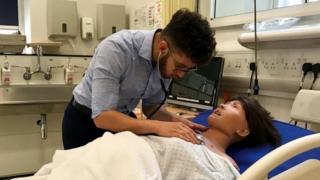
Image copyright
King’s College London
Medical student Yousef El Tawil once thought school was a waste of time
“You’d see people getting stabbed. You’d see people getting robbed for their belongings.”
In 2010, aged 14, Yousef El Tawil, felt “swept into a vortex of pessimism”.
At the end of Year 9, instead of heading home after school to do his homework each day, he fell in with classmates who spent hours hanging around the chicken shops on his local High Street, in Newham, east London.
They weren’t bad people, he says, “it’s just we lacked a certain motivation, we lacked aspirations”.
And they viewed school as futile, “like, ‘There’s nothing for me here,’ and to be fair it was kind of cool to be in that crowd”.
From the beginning of Year 10 Yousef was “on report”, having to be signed off for every single lesson. The attitude was “If he causes any problems, you need to let us know,” he says.
His grades plummeted and his teachers couldn’t get through to him even after one friend was stabbed in the street.
But Yousef’s life changed after an accident in school on the day of his last exam.
He hates talking about what happened but remembers his form tutor urging him not to waste his potential – then “half an hour later, I ended up climbing a very sharp and tall gate at the back of the school” – and it was there the accident happened.
The thumb on his right hand was severed and 10 hours of emergency surgery to reattach it failed when the tissue died.
Yousef’s mum’s reaction in the accident and emergency unit brought him up short.
“She wears a niqab [Islamic veil] and she just looked at me and I could see tears,” he says.
“There’s one thing that I think every person can agree on, whether they’re the harshest human or… the softest, and that’s like when you see your mother go through difficulty, it really touches you, it really makes you think about what you’ve done and reflect.”
That summer, instead of football in the park or evenings with friends, Yousef found himself on the children’s ward at the regional hospital, where he underwent reconstructive surgery.
There were skin grafts, tissue was stretched and blood vessels diverted, there was an infection and he feared he might lose the whole hand.
It prompted a big change.
He says: “After being in hospital for two months, around the doctors, around the nurses, I was like, ‘I want to be part of this. I want to be in that position, to help another Yousef who may have lost a thumb because of a bad decision.’”
Yousef knew he wanted to be a doctor – but how? His Year 10 GCSE exams were a write-off. “I failed everything, except Arabic, my native language,” he says.
Image copyright
Yousef El Tawil
Within a year of the accident, Yousef (top row, third right) was well enough to join his local Sunday league
Under the old-style modular GCSEs, Yousef could resit. He had to do 24 exams in one month – but such was his drive that he achieved 13 A*s, As and Bs.
His teachers still thought his chances of achieving good enough A-levels for medical school were weak and tried to talk him out of it – there are 11 or 12 applications for each place, with entry grades of at least AAA.
But a friend told Yousef about the extended medical degree programme at King’s College London – and he decided to apply there, as well as for standard courses.
He was rejected outright everywhere – except King’s, which interviewed him and made an offer.
When results day brought the grades he needed, he says, “my mum was in tears, I was in tears… it was a huge sense of relief and reward because I had worked so hard to get there”.
The King’s extended course runs for six years, rather than the conventional five and spreads the first year of the medical degree over two years.
There’s individualised extra support where needed, whether academic, pastoral or financial, but students are taught with and take the same exams as students on the standard course.
“It’s about giving them equal opportunity to succeed… they are academically just as capable,” says course co-director Dr Jane Valentine.
Set up in 2001, it was the forerunner of 20 gateway or foundation medicine programmes now run by UK universities.
Medical schools have faced severe criticism that they recruit disproportionate numbers of students from private or selective schools, leading to a lack of diversity in the profession – and these courses are among measures gradually bringing change.
The King’s extended course was initially limited to students with academic potential from non-selective schools in parts of London without a tradition of sending pupils to medical school but since 2017 it has recruited across the UK.
Up to 90% of students are from black and minority ethnic backgrounds, with a similar proportion from households with annual incomes of less than £40,000, predominantly the first in their family in higher education.
Co-director Prof Steve Thompson says the course has the express aim of “levelling the educational playing field”.
It’s “a cornerstone to King’s commitment of giving back to society and it sounds very crass but making the world a better place”, he says.
He is clear that the medical profession should better reflect a population who “aren’t all white middle class”.
“Patients feel more comfortable telling you something if they feel a connection with you,” says Dr Valentine.
“I’m not saying it’s not possible to do that with any good doctor but, you know, there’s no need for it to be full of a certain kind of person.”
- Relax A-level grades for some medical students
- Half of universities have fewer than 5% poor white students
For Yousef, his goal of qualifying as a doctor is in sight, “God willing”.
It hasn’t always been easy, there have been pre-exam panics, even though he’s now in the top 15% of all students across both the standard and extended courses and is about to embark on a master’s degree in global health policy.
“It’s been crazy to be honest,” he says. “I’ve been through a lot. I’ve changed a lot, I would say had ups and downs… I really thank God.”
If he gets the breaks, he says, he would love to work in a hospital serving the area he grew up in.
He feels his Newham roots have given him a richer outlook on life and will, ultimately, make him a better doctor.
He still lives there and sees his friends from school regularly. “It’s still my community, my people and I’m proud of it,” he says.
[ad_2]
Source link








